4,400 Amputations in Australia every year
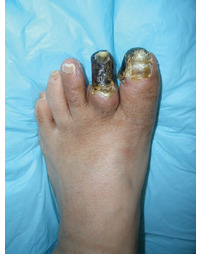
In Australia, there are more than 4400 diabetes-related amputations every year.[i] We have the second highest rate in the developed world.[ii]
Every year there are 10,000 hospital admissions in Australia for diabetes-related foot ulcers in Australia – many of these end with people having a limb, or part of a limb, amputated.[iii] Recent data suggests rates of diabetes-related amputations increased by over 30% between 1998 and 2011 – clearly this is unsustainable.[iv]
Experts estimate diabetic foot disease costs Australia around $875 million every single year.[v] The average cost of a diabetes-related limb amputation is around $23,555, and an additional annual spend of $6,065 every year afterwards. Over five years a diabetes related amputation costs the health system almost $50,000 and that doesn’t include social costs.[vi]
Recent new research suggests investing in evidence-based care for Australians with diabetic foot ulcers could save around $2.7 billion over five years. That is around $9,000 per person aged under 75 and $12,000 per person aged over 75 (both over five years).[vii] Patients with diabetic foot ulcers have morbidity and mortality rates on par with aggressive forms of cancer. Diabetes complications – like diabetic foot ulcers – massively increases the cost of providing healthcare to people with diabetes. For instance, the cost of providing healthcare to someone who has had a diabetic foot ulcer is more than five times higher (5.4) than providing healthcare to someone who doesn’t have a foot ulcer.[viii]
Limb amputations are threatening to bankrupt our hospital system. People with diabetes hospitalised for lower limb amputation have longer stays in hospital than other diabetes- related conditions. The average length of stay is around 26 days.[ix] Research shows it is possible to reduce preventable amputations and hospitalisation by as much between 24 to 90%. [x] Around 85% of diabetes related amputations are preventable if wounds are detected early and managed appropriately.[xi]
A Success Story
In Western Australia the Fremantle Diabetes Study observed a 70% fall in rates of amputation over a 15-year period. This was achieved by ensuring better access to health services including coordinated multidisciplinary care and better education.[xii] Improved models of care have helped drive a 20% reduction in diabetes foot-related hospitalisations and amputations within five years.[xiii]
When a diabetic patient is referred to see a vascular surgeon, it is usually at the end of the road. Unfortunately, by the time a person with diabetes goes to see a vascular surgeon they have already developed limb-threatening complications like ulcerations or infections. A vascular surgeon can work to save their feet through procedures like revascularisation, but this still means that the person with diabetes is facing a long and complex road to recovery. Quite often multiple complex surgical procedures are necessary.
Education is an essential part of diabetes management and people with diabetes should be encouraged and supported to understand the best diabetes management options on offer. This includes everything from food and lifestyle choices to appropriate footwear. Of course, it isn’t always easy. Ongoing diabetes management requires a lot of self-discipline especially in the face of a barrage of marketing and advertising which can make it easier for people to make less healthy choices. It also involves a time commitment which can be tough for some people. Regular check-ups with healthcare professionals take time and effort, and don’t always fit in easily with people’s busy schedules.
In rural Australia, services are limited, and the distances are great. Things like the first visit to a GP and then the referral to a specialist are often delayed. The difficulty in accessing services means that by the time many people with diabetes in rural areas see a specialist they are in the advanced stages of diabetes-related complications.
It is always advisable, if you’re told that you need to have a limb amputated, to get a second opinion.
Vascular teams perform limb saving procedures every week using advanced refinements of a technique known as endovascular revascularisation. This involves passing a wire into the arteries of patients and inflating them with a balloon before inserting a stent that acts like scaffolding to keep the arteries open. This helps improve blood flow and gives the limb a much better chance of survival. There have been significant developments in the field of vascular surgery over the past 20 years. Amputations were more common 20 years ago.The face of vascular surgery has completely changed. With the focus being on a minimally invasive approach to surgery so that they can minimise the risk to patients. Often surgery is performed as a day procedure and there has been a massive reduction in major amputations as a result. People who have a minor amputation will usually go home within a few days.
A review of Prince of Wales Hospital over an eight-year period showed an amazing reduction in the number of major amputations by more than 60 per cent. It reinforces that taking a minimally invasive approach to saving limbs can be as effective, or even more effective, than old open surgery technique
REFERENCES
[i] Australian Commission on Safety and Quality in Health Care, (2016). Australian Atlas of Healthcare Variation. [online] Australian Government. Available at: http://www.safetyandquality.gov.au/atlas/ [Accessed 29 Jun. 2016].
[ii] Bureau of Health Information: Healthcare in focus: how NSW compares internationally. Sydney: NSW Government; 20083
[iii] Davis, W., Norman, P., Bruce, D. and Davis, T. (2006). Predictors, consequences and costs of diabetes-related lower extremity amputation complicating type 2 diabetes: The Fremantle Diabetes Study. Diabetologia, 49(11), pp.2634-2641.
[iv] Lazzarini, P., Gurr, J., Rogers, J., Schox, A. and Bergin, S. (2012). Diabetes foot disease: the Cinderella of Australian diabetes management?. Journal of Foot and Ankle Research, 5(1), p.24.
[v] Based on research from the Australian Diabetic Foot Network.
[vi] Lazzarini, P., Gurr, J., Rogers, J., Schox, A. and Bergin, S. (2012). Diabetes foot disease: the Cinderella of Australian diabetes management?. Journal of Foot and Ankle Research, 5(1), p.24.
[vii] Cheng, Q., Lazzarini, P., Gibb, M., Derhy, P., Kinnear, E., Burn, E., Graves, N. and Norman, R. (2016). A cost-effectiveness analysis of optimal care for diabetic foot ulcers in Australia. International Wound Journal.
[viii] Armstrong, D., Kanda, V., Lavery, L., Marston, W., Mills, J. and Boulton, A. (2013). Mind the Gap: Disparity Between Research Funding and Costs of Care for Diabetic Foot Ulcers. Diabetes Care, 36(7), pp.1815-1817.
[ix] Diabetes. (2008). Canberra: Australian Government, Australian Institute of Health and Welfare.
[x] Australasian Podiatry Council (APodC): Diabetes amputation and hospitalisation reduction program (DAHRP): Budget submission from the Australasian Podiatry Council 2012. Melbourne: Australasian Podiatry Council; 2012.
[xi] Bakker, K., Apelqvist, J. and Schaper, N. (2012). Practical guidelines on the management and prevention of the diabetic foot 2011. Diabetes/Metabolism Research and Reviews, 28, pp.225-231.
[xii] Baba, M., Davis, W., Norman, P. and Davis, T. (2015). Temporal changes in the prevalence and associates of diabetes-related lower extremity amputations in patients with type 2 diabetes: the Fremantle Diabetes Study. Cardiovasc Diabetol, 14(1).
[xiii] Lazzarini, P., O’Rourke, S., Russell, A., Derhy, P. and Kamp, M. (2013). Reduction in the incidence of diabetes lower extremity amputations in Queensland: 2005-2010. Journal of Foot and Ankle Research, 6(Suppl 1), p.O20.
World Diabetes Day is marked every year on 14 November, the birthday of Sir Frederick Banting, who co-discovered insulin along with Charles Best in 1922. Australia has the second highest rate of diabetes-related amputations in the developed world.




